
Health insurance claim rejected by TPA in India is a situation many policyholders face without fully understanding what went wrong. If your claim has been denied by a Third Party Administrator (TPA), it doesn’t necessarily mean the case is closed.
If your health insurance claim was rejected and the reason mentions “TPA decision”, it can feel confusing and frustrating. Many policyholders in India don’t fully understand the role of a Third Party Administrator (TPA) — and more importantly, whether a TPA can actually reject your claim.
The truth is, while TPAs process claims, the final responsibility lies with the insurer. So if your health insurance claim is rejected by TPA in India, you still have multiple ways to challenge and reverse that decision.
Also read: Health Insurance Claim Denied – What to Do
What is a TPA in Health Insurance?
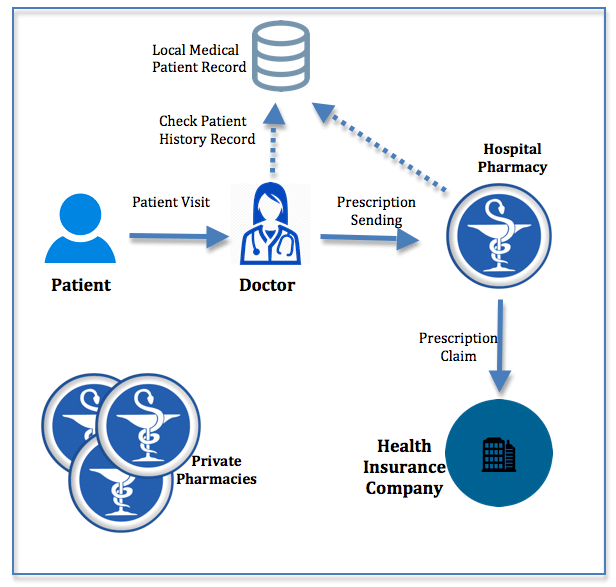
A Third Party Administrator (TPA) is a company hired by your insurance provider to handle claim processing. They act as an intermediary between you, the hospital, and the insurer.
In most cases, TPAs:
- Process cashless approvals
- Verify documents
- Assess claim eligibility
- Communicate with hospitals
However, they do not issue policies or own the final decision legally.
Can a TPA Reject Your Health Insurance Claim?

This is where most people get confused.
While TPAs may communicate the rejection, the decision is technically taken on behalf of the insurance company. This means:
- The insurer is still accountable
- You can directly challenge the insurer
- You are not limited to TPA communication only
So even if your health insurance claim is rejected by TPA in India, it is NOT the end of the road.
Common Reasons for TPA Claim Rejection
Let’s look at real-world reasons why TPAs reject claims:
1. Policy Exclusions
If the treatment falls under exclusions, TPAs may deny approval.
2. Pre-existing Disease Waiting Period
If the illness is linked to a pre-existing condition not covered yet.
3. Documentation Issues
Missing discharge summary, bills, or diagnostic reports.
4. Medical Necessity Doubt
TPA may feel hospitalization was not required.
5. Late Intimation
Delay in informing insurer about hospitalization.
Most of these are procedural and can be challenged.
Related: Common Reasons for Insurance Claim Rejection
Step-by-Step: What to Do If Claim is Rejected by TPA
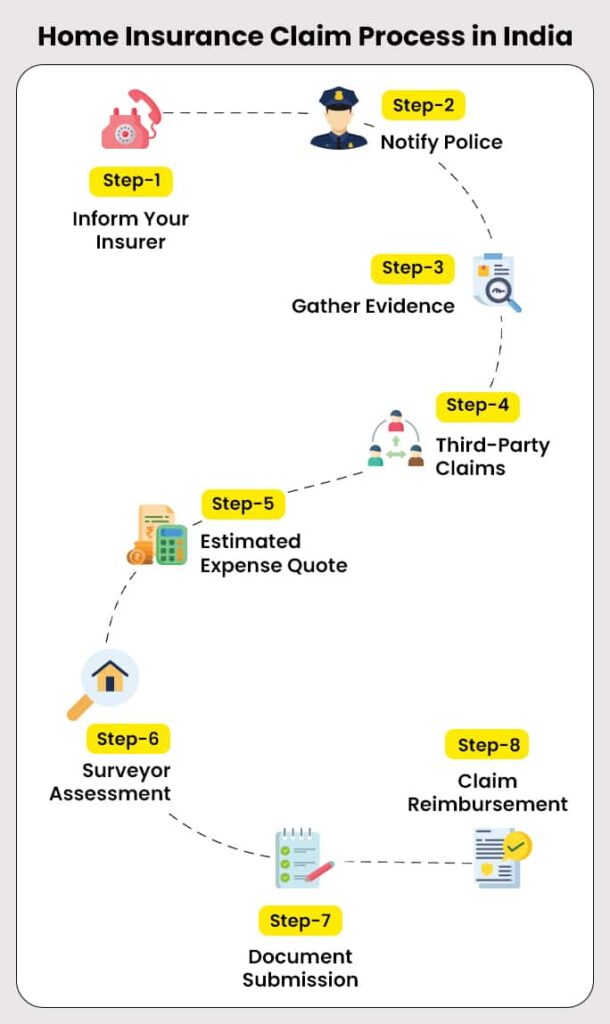
Instead of panicking, follow this structured approach:
Step 1: Get the Exact Rejection Reason
Ask for a written rejection letter. Do not rely on verbal communication.
Step 2: Verify Policy Terms Yourself
Check if the reason is genuinely valid or misinterpreted.
Step 3: Submit Clarification with Documents
Many rejections happen due to incomplete understanding. Submit:
- Doctor’s clarification
- Additional reports
- Revised discharge summary
Step 4: Escalate to Insurance Company
Do not depend only on TPA. Email your insurer directly with all documents.
Step 5: File Grievance
If unresolved, raise complaint through insurer grievance system.
Step 6: Escalate to IRDAI
If still not resolved, escalate to regulatory authority.
Important Tip Most People Miss
Many policyholders keep following up only with the TPA.
This is a mistake.
Always escalate to the insurance company — because legally, they are responsible for claim settlement.
Real-Life Scenario
A policyholder in Pune had a claim rejected by TPA stating “hospitalization not required.”
However, after submitting a doctor’s detailed explanation and escalating to the insurer, the claim was approved within 10 days.
This shows that TPA decisions are not final.
When Should You Escalate Immediately?
- Claim rejected without clear reason
- TPA not responding
- Hospital already discharged patient
- High claim amount involved
In such cases, skip delays and escalate quickly.
Documents You Should Prepare
- Policy copy
- TPA rejection letter
- Hospital bills
- Discharge summary
- Doctor certificate
- All reports
Your Rights as a Policyholder in India
You are protected under regulations by the Insurance Regulatory and Development Authority of India.
- Right to clear rejection reason
- Right to appeal
- Right to grievance redressal
- Right to approach Ombudsman
Why TPA Rejections Are More Common Than You Think
In India, most policyholders assume their insurance company directly handles everything. But in reality, TPAs process a large portion of claims — especially in cashless treatments.
This creates a gap.
TPAs follow internal guidelines and documentation checks very strictly. Even small issues like unclear handwriting in medical notes, missing investigation reports, or slight mismatch in diagnosis can lead to rejection.
And here’s the important part — many of these rejections are not final decisions, but temporary outcomes due to lack of clarity.
That’s why understanding how to respond becomes more important than the rejection itself.
Difference Between Cashless and Reimbursement Rejection by TPA
The experience of rejection can vary depending on the type of claim:
Cashless Claim Rejection
This usually happens during hospitalization. The TPA denies approval, and you may be asked to pay from your pocket.
In such cases:
- You can still file for reimbursement later
- You should collect all original documents
- You must inform the insurer immediately
Reimbursement Claim Rejection
This happens after treatment when you submit documents for repayment.
Here, rejection is often due to:
- Missing bills
- Incomplete documents
- Policy condition misunderstandings
Compared to cashless, reimbursement claims have a higher chance of correction if you respond properly.
Common Mistakes People Make After TPA Rejection
Many policyholders unknowingly reduce their chances of approval by making these mistakes:
- Accepting rejection without questioning
- Not asking for written justification
- Failing to submit additional medical proof
- Delaying escalation to insurer
- Not keeping copies of documents
Avoiding these mistakes alone can significantly improve your chances of claim approval.
How to Write a Strong Reconsideration Request
If your health insurance claim is rejected by TPA in India, your response should be clear and structured.
Your email or letter should include:
- Your policy number and claim number
- Clear mention of rejection reason
- Your explanation against that reason
- Supporting documents from doctor or hospital
- Request for re-evaluation
Keep your tone professional and factual. Avoid emotional language — focus on medical and policy justification.
Timeline You Should Follow After Rejection
Time is critical in insurance matters.
- Within 24–48 hours: Collect rejection details and documents
- Within 3–5 days: Submit clarification to TPA and insurer
- Within 7–10 days: Follow up and escalate if no response
- Within 15–30 days: File grievance if unresolved
Delays from your side can weaken your case, especially in reimbursement claims.
Pro Tip: Always Keep the Insurer in Loop
Even if the TPA is handling your claim, always mark a copy to your insurance company in emails.
This ensures:
- Transparency
- Faster escalation
- Accountability
Many claims get resolved faster when insurers are directly involved instead of relying only on TPA communication.
Step-by-step guide: How to Appeal Insurance Claim Denial in India
Final Thoughts
If your health insurance claim is rejected by TPA in India, don’t assume your claim is permanently denied.
In many cases, claims are approved after clarification or escalation. The key is to act quickly, understand the reason, and challenge it with proper documentation.
To conclude, if your health insurance claim rejected by TPA in India situation arises, remember that it is not a final decision. With proper documentation, timely action, and escalation, many claims can still be approved successfully.
Remember — TPA is just a processor, not the final authority.
